‘No way back’: Performing euthanasia in the Netherlands
When somebody wants to die in the Netherlands, Bert Keizer is often the man they call.
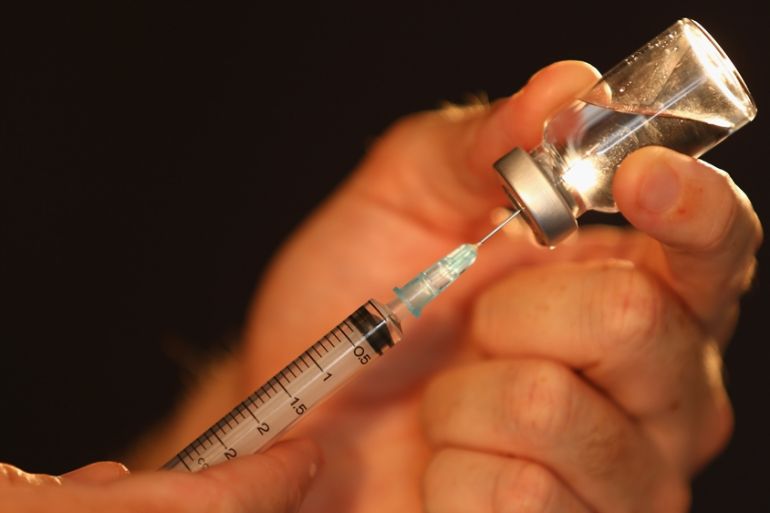
About once a month, Bert Keizer gets a phone call from the clinic where he works. Somebody wants to die – the voice at the other end of the line will say – is he available to go and see if that request can be granted?
Keizer, a Dutch geriatrician, works for the End of Life Clinic (Levenseindekliniek) which offers euthanasia or assisted suicide to people whose own physician has denied their request.
Keep reading
list of 4 itemsGaza lost much more than a hospital when it lost al-Shifa
With measles on the rise, rebuilding trust in vaccines is a must
Could a bird flu pandemic spread to humans?
Last year, Keizer received 22 such calls. He granted 16 of the requests and performed the euthanasias himself.
For every case that comes in, Keizer will meet the patient several times before deciding if he or she is eligible for euthanasia. Then, a second doctor has to meet the patient and agree with Keizer’s decision.
Only then can Keizer carry out the euthanasia. He prefers using a nervous system depressant called a barbiturate which the patient drinks, causing them to die within 10 to 15 minutes. If that isn’t a good option, because the patient can no longer swallow as a result of their illness or they are afraid of nausea, Kaiser administers an injection.
‘There’s no way back’
Keizer, who worked in a nursing home for 34 years before retiring and joining the End of Life Clinic, remembers his first euthanasia vividly.
“It was 1984. Euthanasia wouldn’t be legal for a long time, so you had to work in a sort of clandestine way and that led to all these idiotic manoeuvres. This patient was living in the nursing home where I worked, so it’s not like I could shout down the hall, ‘Mr so-and-so is going to die tonight’. I got the right medication and I administered it wrong. I was dead nervous,” Keizer recalls.
“There are two things you fear when you perform a euthanasia,” he continues. “One is that it works, in which case you’ve got a dead person. The second fear is that it doesn’t work, in which case you’ve got a living person who wants to die.”
While performing a euthanasia no longer keeps Keizer up at night, he says it still takes a toll. “It’s a huge responsibility, because you know there’s no way back,” he reflects. “It’s not like you can ask after the procedure, ‘So, this is definitely what you wanted?’ That’s a tortuous aspect about euthanasia. I never do it without fear.”
In part, Keizer’s drive to work for the End of Life Clinic stems from something he calls “investing altruism”: “It’s about looking ahead to the bad stuff that might happen to me someday, and feeling reassured that people will help me instead of telling me I’m just going to have to sit it out.”
But for the most part, his motives are surprisingly practical: he’s retired and wants to keep busy. “After solving my crossword puzzle, I want to leave the house,” he says.
A legal practice
Euthanasia has been enshrined in Dutch law since 2002. When a patient who is experiencing unbearable suffering with no prospects for improvement has asked to die, it is legal for a doctor to administer a fatal dose of medicine, or supply the patient with it for them to take it themselves.
Every doctor has the right to refuse a euthanasia without stating a reason. Patients can then try again at the End of Life Clinic where Keizer works.
After a euthanasia happens, a review determines if the doctor has abided by the rules. Failing to do so would result in criminal prosecution and a prison sentence of up to 12 years.
On September 28, Dutch public prosecutors started a criminal investigation, for the first time since the law came into effect, into a doctor who performed a euthanasia. Reviewers had determined that the doctor did not act according to the rules when she administered a deadly dose of medicine to a 74-year-old woman suffering from severe dementia.
Over the years, Dutch euthanasia legislation has attracted a lot of international press coverage, fostering the idea that dying by appointment is widespread in the Netherlands. But this is a far cry from reality. In 2016, there were 6,091 instances of euthanasia reported to the regional evaluation committees – less than five percent of the nearly 150,000 people who died in the Netherlands that year.
A personal choice
Christiaan Rhodius is a medical doctor who has focused on palliative medicine for the past 10 years. Unlike Keizer, he has never performed a euthanasia.
In the hospice where he works, there aren’t all that many requests to begin with, he stresses. Many patients wanting euthanasia would have asked their GP about it before getting to a palliative care facility. But personal misgivings have also played a part.
“Initially, I thought I just couldn’t do it, deliberately taking the life of someone else. I’ve also asked myself if as a human being I have the right to end the life of another human being, even if it’s explicitly requested,” Rhodius explains.
“Now, I notice that there are situations where I think the idea of mercy outweighs the duty not to harm a patient.”
Rhodius has started the euthanasia procedure twice. In one case, the patient ended up dying naturally anyway. The second time, the patient changed his mind, which is something that Rhodius says is not uncommon.
There's two types of fear of death: the fear that it will be ugly and painful, and there's the fear of no longer being there.
In Rhodius’s view, there’s no such thing as a right to euthanasia.
“Because a right presupposes a duty and that means that I as a doctor have to comply,” he says. “As a doctor, you have to be convinced that having mercy outweighs the principle of no harm in each case. Each doctor finds his own path in this, based on a different belief system.”
For Keizer, there are two types of cases which he refuses to approve. One is when an older person who is relatively healthy asks for euthanasia because they feel they’ve had a long enough life. “You can think that, but to me that doesn’t mean you should get the help of the state or a doctor – you’ll have to arrange it yourself,” he says.
He also draws the line at people who suffer from dementia to the point that they can no longer give verbal approval – even if they’ve previously put their desire to die in the case of dementia on paper. “I’m not going to participate in that,” Keizer says.
His experience with death throughout his career has changed his outlook on his own.
“There’s two types of fear of death: the fear that it will be ugly and painful, and there’s the fear of no longer being there,” he says.
“The second one, that more philosophical fear, is as strong as ever in me. I’m not religious and I don’t think there’s an afterlife – and I’m not happy about that. But that first fear has improved a lot. I think that dying is something that can be managed quite well.”
|
|
