Pakistan’s polio puzzle
Why does Pakistan continue to suffer from polio, despite billions of dollars spent on eradication programmes?
The basic idea that lies behind the eradication of communicable diseases, including polio, was that with enough funding, technology and organisation, they could be eliminated. This philosophy managed to wipe out smallpox, and had enough success to inspire confidence that no other tools or ideas were needed. It is now all too clear that funding, technology and organisation are not the whole puzzle. Just visit polio’s 21st century ground zero, Pakistan, from where the disease threatens not just the country itself but also its neighbours and other countries which had been polio-free for years.
In Pakistan, where 66 cases of polio have already been diagnosed this year, the inadequacy of that fundamental idea has been exposed. Pakistan has had access to all the available science and technology; it has experimented with different organisational methods; and it has had access to massive amounts of funding to combat polio from donor governments, private organisations and others – including, recently, $20m from Canada, $251m from the Islamic Development Bank, and more than $85m between 2001 and 2011 from the Bill and Melinda Gates Foundation.
They continue to offer more, as if hoping that one more dollar will make the difference in a country where vaccine coverage rates have rarely risen above 50 percent and where the long-standing issues in procurement, transport, cold-storage systems and coordination are familiar and accepted parts of the equation.
Conventional wisdom now offers a convenient excuse for Pakistan’s failure to remove polio: Service-delivery challenges, such as the horrifying attacks on polio workers, and increased militancy and unrest throughout the country need to be addressed through the holy trinity of funding, technology and organisation. The situation has grown more challenging, but focusing attention on these new and immediate issues only helps to obscure the deeper underlying problem that has been present from the beginning.
|
|
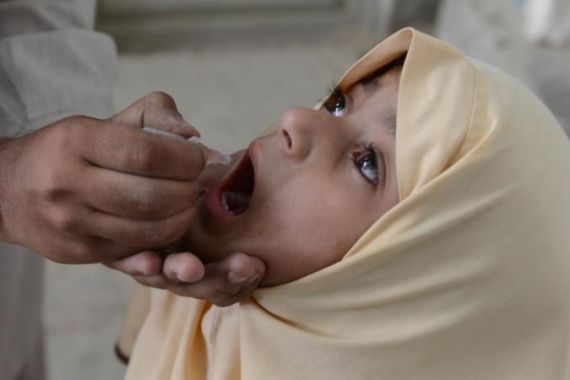
| Life Lines – The Last Drop |
What’s been missing in Pakistan for so many decades is an understanding of the big picture – which means, in part, acknowledging that funding, technology and organisation do not exist in a vacuum, but are applied in particular ways to particular contexts.
If increasing amounts of funding, steadily developing science and modified organisational plans have consistently failed, the only logical step is an analysis of the context. To use a medical analogy: There is pathology here, and increasing doses of the old medicine have not worked. Before upping the dose again or changing the prescription, the disease has to be diagnosed.
The best place to look is in the design and implementation strategy of the polio-eradication programmes to which all the funding, technology and organisation have been applied. Pakistan’s Polio Eradication Programme was designed three decades ago and has not changed since.
It is now outmoded and radically out of sync with the local context. It is rigidly structured and inflexible, unable to respond to challenges either in the field or at the policy level. Management responsibility has been divided between United Nations agencies, non-governmental organisations, and the government – yet there are still significant overlaps between the tasks of the provincial and central government. Thus these efforts are uncoordinated and no one is truly accountable.
Mistakes repeated
In the past few decades, repeated trials of the same programme have replicated the same mistakes at each step. Donors prioritise how much money is spent, rather than how effectively it is spent – and in any case, there are many donors, NGOs and other agencies competing over the same turf. Inadequately trained staff are hired only for intensive campaigns of a few days, and therefore – despite the best of intentions and despite the incredible courage that has become increasingly necessary for them – they are poorly informed and not invested in the programme’s overall success.
There is rarely any attempt to communicate effectively to the recipient population about the vaccinations. At best, printed brochures are distributed, but given that literacy rates are low in many of the at-risk communities (the literacy rate for women is barely above 50 percent in Punjab and is less than half that in Balochistan), these are largely useless.
The inability to even properly inform the population reflects a more disturbing problem: That polio eradication in Pakistan has consistently treated the recipients as little more than passive and recalcitrant targets. Their context has been brushed aside entirely, in a trend that is only growing worse. The dollars, the technology and the organisational changes are closely examined – but no one takes more than a glance at the men, women and children who are meant to benefit from them. There is, of course, no space for communities to have a say in the programmes themselves – no one has even thought to ask them the basic questions.
Addressing basic issues
So let’s ask some basic questions.
What do these people know? Research about those who resist the measles vaccine, for example, has demonstrated that simply providing information is not effective in creating demand. A UNICEF-sponsored survey in 2012 found that in 29 high-risk districts in Pakistan, 46 percent of respondents were not aware of vaccinations against polio.
What do they understand? (Working in Sindh and Khyber-Pakhtunkhwa in the past, I found many families who saw drops and injections as medical interventions only necessary when someone was already sick; there was no concept of prevention.) What are they afraid of? What is important to them? Why do they make the decisions they make? What is the daily reality of their lives on which all our money and science and programme managers are meant to have an impact?
Until these questions are sincerely asked, and until the answers are seriously considered, the puzzle will remain incomplete and polio will continue to cripple the nation’s children. Without this understanding reflected in a subsequent contextual, programme design and implementation strategy, future vaccination efforts, even if generously backed by public and private donors, are likely to meet the same fate as the previous ones.
Dr Samia Altaf, a public health physician, was the 2007-08 Pakistan Scholar at the Woodrow Wilson Center in Washington, DC. She is the author of So Much Aid, So Little Development: Stories from Pakistan published by the Johns Hopkins University Press in 2011.
