Healthcare workers across Africa share their coronavirus stories
Doctors and nurses from across the continent recount experiences of fighting the COVID-19 pandemic on the front lines.

With the number of confirmed COVID-19 cases rising in many African countries, healthcare workers across the continent have been at the forefront of the response to the disease.
As in other parts of the world, many of these doctors and nurses are confronted with challenges in the face of the coronavirus pandemic sweeping the globe, while others remain optimistic about the systems within which they operate.
Keep reading
list of 4 itemsMexico’s teachers seek relief from pandemic-era spike in school robberies
‘A bad chapter’: Tracing the origins of Ecuador’s rise in gang violence
Why is the US economy so resilient?
Here, they share their stories of fighting the pandemic on the front lines. Some have chosen to remain anonymous.
Dr Bernard Hammond, president of Ghana Association of Doctors in Residency, Komfo Anokye Teaching Hospital in Kumasi, Ghana
With more confirmed cases every day, most of us are apprehensive about the availability of personal protective equipment (PPE). There has been a general shortage of basic protective equipment like facemasks, leading to reuse and prolonged use by health staff.
We are, however, quite resolute in fulfilling our duties, even in times like these.
The government’s announcement that health workers will be exempt from paying taxes for three months and a 50 percent salary raise for those who routinely come into contact with confirmed cases have indeed served to boost morale. Our concerns regarding equipment also seem to be generating some favourable response from the government, evidenced by their promotion of the local manufacturing of PPE and other logistics to meet our needs in the clinical setting.
The government has established health insurance packages for healthcare workers and protocols have also been established at the facility level for the isolation and testing of any staff exposed in the line of duty. During the period of isolation, arrangements have also been made for them to be taken care of.
COVID-19 in Ghana (as of April 29) – Confirmed cases: 1,671 – Recoveries: 188 – Deaths: 16

Dr Olusegun Olaopa, former president of Nigerian Association of Resident Doctors – University College Hospital in Ibadan, Nigeria
Healthcare workers in Nigeria face challenging working conditions with no life insurance, inadequate pay and constant burnout. Thus, this pandemic has put more pressure on an already overwhelmed workforce already struggling with low morale.
With the spread of the virus, it is not enough to only provide protective equipment to those at the isolation centre, we need some form of it at all hospitals. Particularly because some doctors in the country that have been exposed to the virus were treating patients who had other ailments and had not been diagnosed with COVID-19. Meanwhile, politicians are using sophisticated protective gear.
We just need encouragement and appreciation so that we know our sacrifices will not be in vain. My department, which is a surgical specialty, has started adopting self-help to adapt makeshift protective materials.
On a positive note, the government has done well in raising awareness, closing borders and imposing a lockdown in three states. The Nigeria Centre for Disease Control is also working tirelessly to ensure the pandemic is being contained.
COVID-19 in Nigeria (as of April 29) – Confirmed cases: 1,532 – Recoveries: 255 – Deaths: 44
|
|
Professor Moussa Seydi, head of infectious diseases department, Hospital Center University De Fann in Dakar, Senegal
The COVID-19 response unit has been well catered for, as the government provided us with enough equipment which they had procured in time. We also received sufficient training and instructions on procedures to follow.
Thus, here in the treatment centre, we feel safe. If we see a huge surge in cases then perhaps this could change.
I believe the government really has done its best; they also announced that healthcare workers will be given bonuses which many of them have already received.
COVID-19 in Senegal (as of April 29) – Confirmed cases: 823 – Recoveries: 296 – Deaths: 9
Doctor in Bamenda, Cameroon
Authorities have done very little in ensuring our safety. Many districts in Cameroon have not received sufficient training, educational materials and PPE.
I learned about safety procedures online, however, many healthcare workers do not have access to the internet. Health workers also do not have access to priority testing – this is both dangerous to them and their patients.
As I speak, official figures suggest at least five doctors have died of the 44 deaths related to COVID-19.
No pay or extra financial support, coupled with constant power cuts at some hospitals, means morale is very low.
COVID-19 in Cameroon (as of April 29) – Confirmed cases: 1,806 – Recoveries: 915 – Deaths: 59
|
|
Public health official in Liberia
The government partially considered the safety of health workers but there has been little commitment to see this through.
For example, health workers have not received hazard pay for months and many are demotivated and even considering strike action or quitting.
One front-line responder died after contracting the virus and we are yet to get any information regarding an insurance package which was supposedly set aside for the family.
COVID-19 in Ghana (as of April 29) – Confirmed cases: 141 – Recoveries: 45 – Deaths: 16
Carol, a hospital nurse in Dar Es Salaam, Tanzania
I am horrified at the lack of action taken by the government – little direction, no transparency, they have refused to implement measures like lockdowns or close places of worship.
As front-line workers, we are simply being ignored and it is terrifying. We are being treated like collateral damage.
COVID-19 in Tanzania (as of April 29) – Confirmed cases: 480 – Recoveries: 167 – Deaths: 10
![Members of a privately-funded NGO working with county officials wearing protective carry their gear during the dusk-to-dawn curfew imposed by the Kenyan Government [Luis Tato/AFP]](/wp-content/uploads/2020/04/acd749288ee641d8a281870673f91479_18.jpeg)
Dr Thuranira Kaugiria, secretary-general of Kenya Medical Practitioners, Pharmacists and Dentists’ Union, Nairobi branch, Kenya
To give credit where credit is due, an isolation and treatment facility for healthcare workers has been set up at Kenyatta National Hospital and the Kenyatta University Teaching Research and Referral Hospital in Nairobi.
Furthermore front-line workers at these hospitals that have been in contact with COVID-19 patients – from security staff to doctors – are being tested. This is also the case at Mombasa Coast General Provincial Hospital.
But it is not enough, the government has taken the PR path. They thank us in their speeches, but where is the PPE? Why are healthcare workers being harassed during curfew hours? When will we have comprehensive medical cover?
COVID-19 in Kenya (as of April 29) – Confirmed cases: 384 – Recoveries: 129 – Deaths: 14
Mary, a hospital nurse in Nairobi, Kenya
A month ago, we downed tools at my hospital due to a lack of training. This has since been rectified.
Last week, President Uhuru Kenyatta announced a welfare package for healthcare workers – I’m sure it is in good faith but the politicians in this country have never appreciated us.
Regardless, we are committed to our jobs and to dealing with this pandemic.
Perhaps COVID-19 will finally lead to people valuing us; perhaps they will remember that we sign up to save lives – we don’t sign up to kill ourselves in the process.
|
|
Surgical registrar in Harare, Zimbabwe
The relationship between this government and medics in the country has never been good, with many of us on strike since November 2019.
Ultimately, even during this pandemic, the government has shown us it does not care.
Earlier this month, the High Court ruled that the government must provide PPE for healthcare workers, yet many still do not have it. In March, we called for sufficient risk allowance and their $37 response was laughable.
There is no screening or priority testing for healthcare workers, and neither is there any insurance package.
My wife and I are both doctors, we have two young daughters and sometimes you wonder whether going to work is even worth the risk. At this point it feels like a choice – don’t go, don’t get paid and die from starvation; go, contract the virus and risk dying from that.
COVID-19 in Zimbabwe (as of April 29) – Confirmed cases: 32 – Recoveries: 5 – Deaths: 4
Junior doctor at a COVID-19 ward in South Africa
My hospital is better off than many others, yet I can’t say I feel fully safe as I am concerned that as cases rise so will the shortage in equipment. This is something we are already seeing in the country.
Already between four of my colleagues and I, we only have three special visors which we share and reuse. Also, on the ward, there are often only two or three doctors dealing with very sick patients who have to wait 48 hours to get their results, and this is overwhelming.
The government’s decision to enforce a lockdown and ban sales of alcohol was a good move on their part, though due to socio-economic factors the lockdown has meant there are people who are really suffering.
COVID-19 in South Africa (as of April 29) – Confirmed cases: 4,996 – Recoveries: 2,073 – Deaths: 93
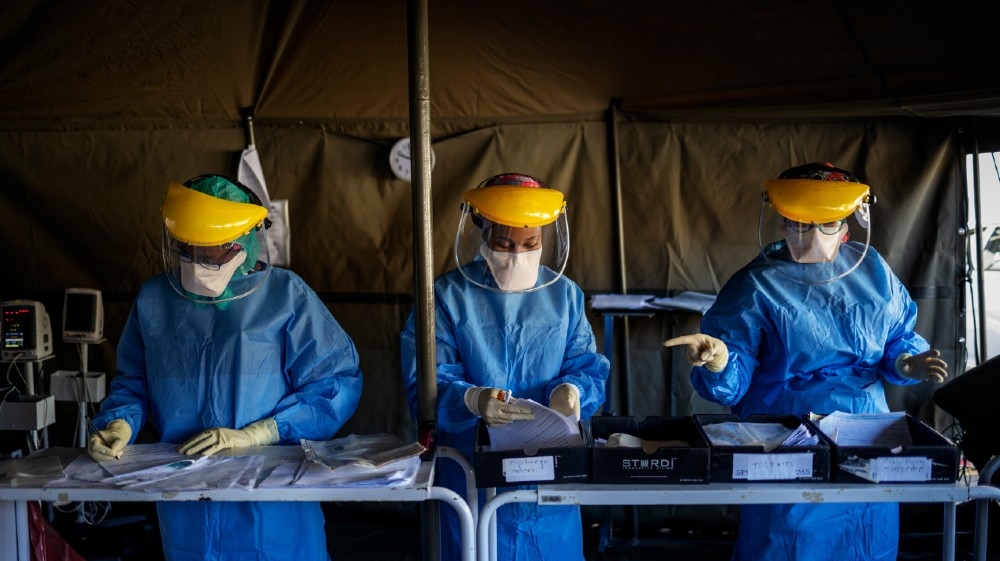
Junior doctor at surgical ward in South Africa
As soon as the country reported its first cases, authorities were quick to provide the hospital with information regarding how the outbreak would be managed.
In terms of front-line workers, as soon as you enter the hospital, you are screened and your temperature is checked. If you feel even one of the symptoms, they test you and send you home and our results are fast-tracked, so we get them within 24 hours.
One big concern is the impact this situation can have on the mental health of front-line staff, especially those that have to isolate from family or live alone.
Some of the interviews have slightly been edited for brevity