On the coronavirus front line: The life of a New York City doctor
Thousands of US healthcare workers spend entire shifts battling COVID-19. ER Doctor Cleavon Gilman is one of them.

A lonely waiting-room chair sits in a quiet hallway between the ambulance bay and the trauma room at a hospital in New York City’s Manhattan borough. This is where Dr Cleavon Gilman goes to make the phone calls he dreads most.
“They know when I call them up, what I’m about to say next,” he tells Al Jazeera. “I say that your [loved one] has died, and it’s almost like, a shock first: ‘What?’ And then this shrill cry and sobbing on the phone.”
Keep reading
list of 3 itemsUS doctors, nurses on coronavirus front line beg for critical PPE
Coronavirus: Overwhelmed US funeral homes turn families away
With COVID-19 mercilessly ripping through New York City, the US epicentre of the deadly global pandemic, Gilman is making these calls more frequently than ever before. The most difficult moment, Gilman says, is actually when he hangs up the phone – and he must get out of the chair, leave the hallway, and go back to treating dozens of other sick patients fighting the infectious respiratory disease.
“That’s the hardest point,” the 40-year-old says, “resetting and knowing that I have to take care of 30 other patients who are all critically ill, too.”
Thousands of healthcare workers are on the front lines of the COVID-19 response in New York City. Several have gone on social media to share their experiences and fears, and to call on people to stay home to try to stem the spread of the novel coronavirus that has so far killed more than 21,000 people in the US, including more than 6,800 in New York City alone.
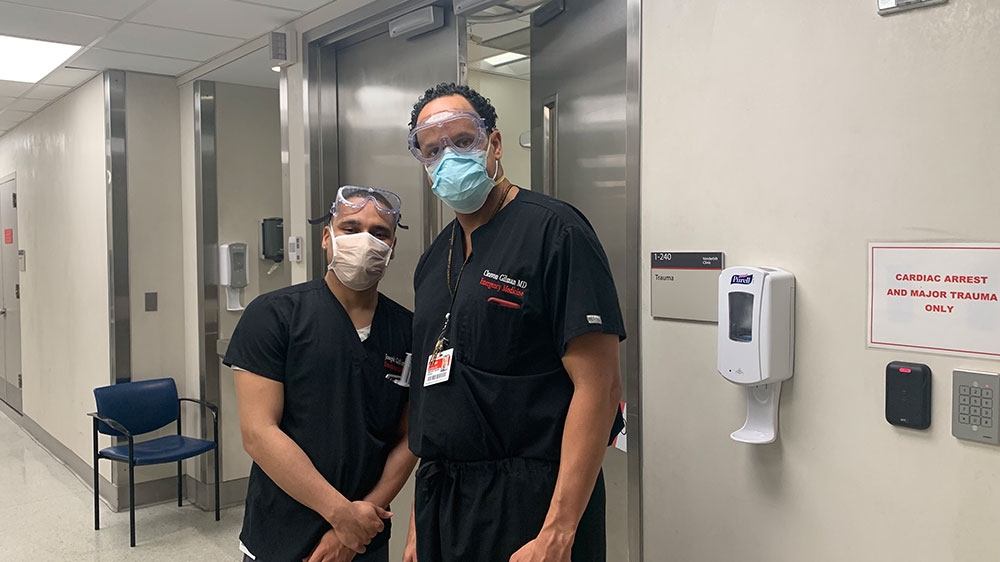
This is the day in the life of one: Dr Cleavon Gilman, senior resident in emergency medicine in New York City.
The start of the shift: Assessing the ‘war zone’
Already dressed in his black scrubs, Gilman’s day starts as soon as he walks through the doors.
“I live a block from the hospital, so I walk over,” says Gilman. First, he scans the waiting room to “gauge how crazy it’s going to be” on his shift, which typically ranges from eight to 12 hours. “I grab my N95 mask, and I put that on. I put on my goggles and a surgical mask, as well.”
Over the past few weeks, more and more people have been coming into the emergency room needing oxygen to breathe, he says, and some days, the number of critically ill patients can reach 80 people.

“Usually there are tens of patients in the hallways with masks on, coughing, hooked up to oxygen,” says Gilman. They are waiting for beds in the intensive care unit upstairs.
Gilman, who spent six years as a medic in the US military, including in Iraq, said the scene is a familiar one, albeit one he had not seen before in New York. “It looks like a war zone nowadays in the hospital.”
The outgoing team of doctors sign over the patients to Gilman and the colleagues he will be working with that day. Usually, there is an attending physician, a senior resident (Gilman, in this case), and two junior residents on shift together, in addition to nurses, technicians and other hospital staff.
The shift: Ebbs and flows
To him, time at the hospital ebbs and flows: it might be slow one minute, and then three critically ill patients will crash at the same time.
Gilman says it has become crucial to know which patients are DNR or DNI: Do Not Resuscitate or Do Not Intubate.
The intubation process is much more invasive than many realise – patients are poked and prodded – and he says intubation has not helped most patients over the age of 75. While patients of all ages have come to the hospital with COVID-19 symptoms, people 65 years and older struggle the most.
“What’s so hard about this is that a lot of these patients were doing well in life. If they had chronic diseases, if they had heart failure, [if] they had asthma, it was well-controlled. They were living into their 80s … and then all of a sudden a virus comes, and it just overtakes them,” says Gilman.
Before a breathing tube is inserted, patients are put under and their airway is paralysed. “That opens up the vocal cords and allows us to put the breathing tube in,” he explains.
The tube is then attached to a breathing machine, which is set to the right level based on a patient’s blood sample. “A breathing machine has to have certain values in it. For example, how many times are you going to breathe a minute? How large are the breaths going to be? How much oxygen am I going to give you?” Gilman says.
“I’m doing this every day; two to three times a shift. It just weighs heavy on the heart.”
He had a 70-year-old patient this month who came into the ER with a piece of paper.
“It said, ‘My husband is hospitalised with the coronavirus, and I also have a fever.'” Gilman contacted the woman’s daughter to let her know that her mother was at the hospital. The woman was placed on oxygen. Within three days, she had passed away.
“I treat every patient as if they’re my mom, they’re my dad, they’re my brother. I got her a blanket, I tucked her in,” Gilman says. “I’m just coming to appreciate that for many of these patients who are older, we’re not going to prevent them from dying from the virus, and I just want to make their last days on this earth as comfortable as possible.”
Real updates from an ER doctor & Iraq War veteran on the frontlines of the coronavirus pandemic in New York City. I tell it like it is… the virus affects all aspects of our society. #CleavonMDjournal @SteflonMD @Craig_A_Spencer @DrTsion @darakass @choo_ek @BetoORourke pic.twitter.com/LJDFoGReDX
— Cleavon MD (@Cleavon_MD) April 3, 2020
Another patient, a 90-year-old man with a history of heart failure who was otherwise independent, came in complaining of shortness of breath. It turned out he did not have COVID-19, but he later contracted it while in the hospital. He died.
Gilman intubated another elderly patient who was not doing well. Before the procedure, he called the man’s daughter to let her speak to her father. “I got my cell phone, I pressed it up against his ear, and she was able to talk to her dad. He was about 60 years old and otherwise healthy, and just having a hard time breathing, so we had to intubate him.”
The end: Deja vu
The moment a patient takes a turn for the worse is especially difficult because that is when Gilman needs to contact the next of kin. Going to sit in the chair in the quiet hallway is both a way to focus on the conversation at hand and hide his own emotions. “What’s helped is, I think, going home and processing and writing in my journal,” he says.
Gilman posts some of his journal entries on Facebook, too. He writes about his work at the hospital, conversations he has had with colleagues, patients and their families, and his own feelings about what is going on around him.
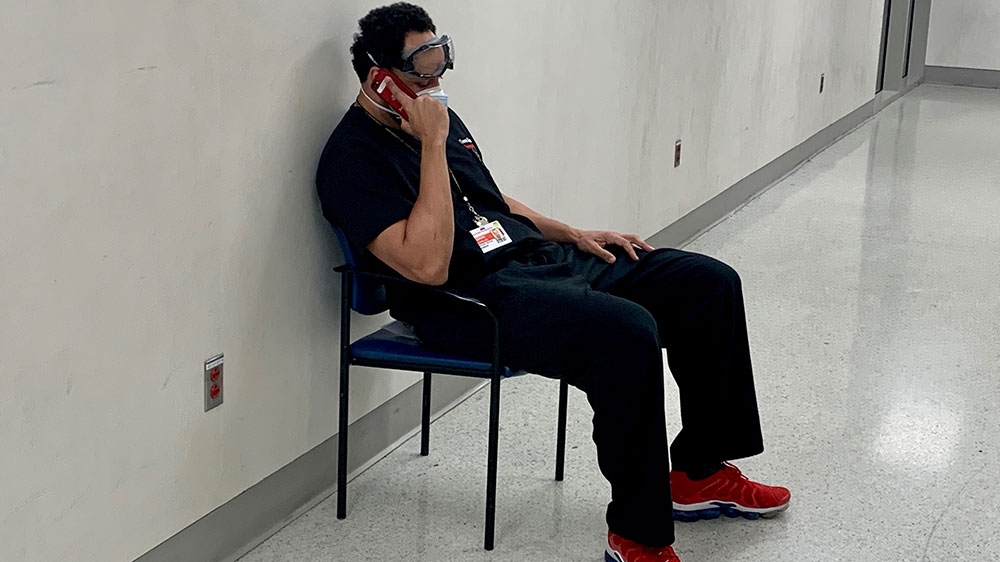
In one post, he described delivering terrible news to the daughter of a woman who had died.
“I could hear her begin to sob through the phone, then she let out a heart-wrenching shrill cry,” he wrote.
“Another piece of me chipped away,” he added. “How many others have used this chair to deliver bad news that their loved one has died from the coronavirus?”
Recently, Gilman finished a particularly difficult day at the hospital, and the one-block walk home became difficult, too. His head was down, his eyes were filled with tears, and it was raining. The virus is taking an emotional toll on him, he admits.
“I’m the only one here at bedside,” he says, and telling families that their loved ones are dying never gets easier.
“They [the calls] get worse. I’m like, ‘Oh my God, I’m doing this again,'” he says. “It’s like deja vu.”