Second confirmed Ebola patient in DR Congo’s Goma dies
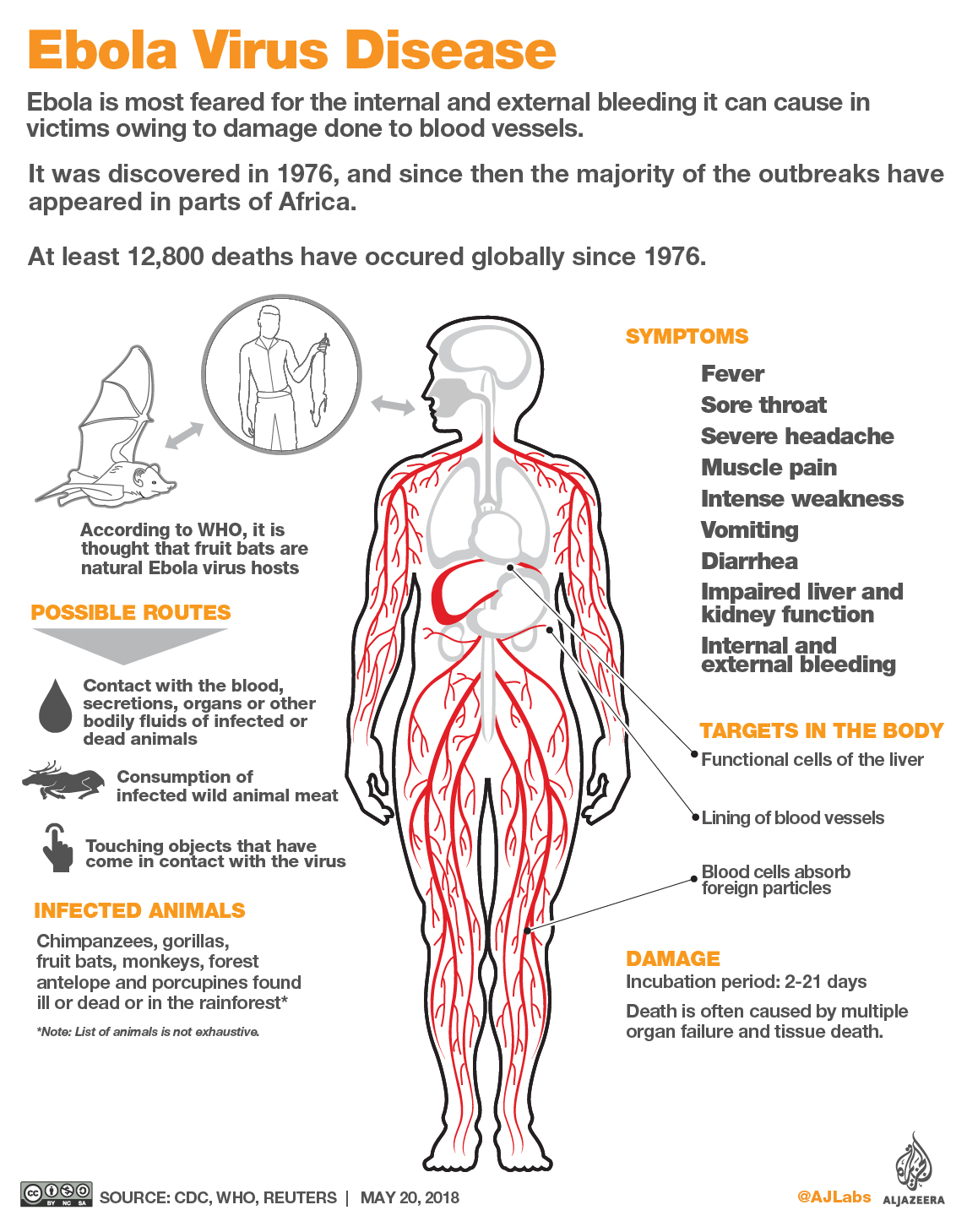
Death of man diagnosed in major transport hub heightens fears the disease could spread beyond DR Congo’s borders.

The second patient to be diagnosed with Ebola in the eastern Democratic Republic of Congo‘s largest city, Goma, has died, according to officials.
Jean-Jacques Muyembe-Tamfum, DRC’s Ebola response coordinator, confirmed the death on Wednesday, a day after the case was announced.
Keep reading
list of 4 itemsWoman, seeking loan, wheels corpse into Brazilian bank
UK set to ban tobacco sales for a ‘smoke-free’ generation. Will it work?
Poland lawmakers take steps towards liberalising abortion laws
“A patient who was confirmed with Ebola in Goma has died. Every measure has been taken to block the chain of transmission,” Muyembe-Tamfum said.
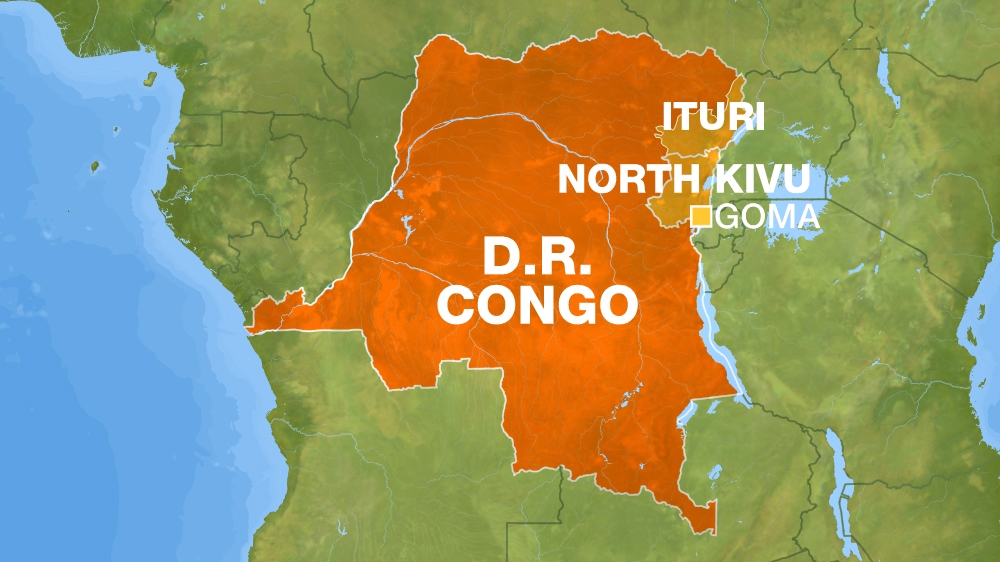
The incident has increased fears the virus could take root in the densely populated city of around two million. Goma is more than 350 kilometres south of where the outbreak was first detected.
Experts warned that the latest incident could accelerate the spread of the disease, which has killed over 1,800 people over the past year and became the second-worst outbreak on record.
|
|
In a joint statement hours after the death was confirmed, several United Nations agencies expressed concern over, saying: “This latest case in such a dense population center underscores the very real risk of further disease transmission, perhaps beyond the country’s borders.”
On Thursday, neighbouring Rwanda closed its border with the DRC because of the outbreak, Olivier Nduhungirehe, Rwanda’s state minister for foreign affairs told The Associated Press news agency.
The Congolese presidency confirmed the closure in a statement, saying there had been a “unilateral decision by the Rwandan authorities” to shut the border for all people other than Congolese citizens leaving Rwanda. It called the decision “regrettable” and said it ran counter to the advice of the World Health Organization (WHO).
Aruna Abedi, who is coordinating the Ebola response in North Kivu, the worst-hit province, said the second patient to die from Ebola in Goma had arrived at a treatment centre “11 days after falling ill”.
“His was really a hopeless case because the illness was already at an advanced stage and he died overnight on Tuesday.”
Abedi urged the public to respond swiftly to symptoms of Ebola and “not hide suspect cases”.
“The treatment centre is not a dying room – you have to bring the patient in early,” he said.
Public health emergency
The man who died was a miner in his 40s returning home from an area of northeastern Ituri province where no Ebola cases in this outbreak have been recorded, WHO officials told reporters.
He could have been exposed to Ebola anywhere between Komanda in Ituri and Goma, as he took moto-taxis over a number of days through the densely populated region at the heart of the outbreak, said Dr Michael Ryan, emergencies chief at WHO.
The man arrived in Goma on July 13 and started showing symptoms on July 22. He was isolated at an Ebola treatment centre on Tuesday. He had spent five days being treated at home and then went to a health facility, where Ebola was suspected.
“He may not even have been aware of the exposure that he had,” Ryan said, adding that the man’s potential contacts were being identified and given an experimental but effective Ebola vaccine.
Symptoms such as fever can be confused with malaria, which is endemic in the region.
Goma’s first Ebola case was detected in mid-July. After his death, the WHO declared the outbreak a “public health emergency“, a move designed to step up the global response.
Health officials said the second case was not connected to the first patient in Goma who was a pastor who became infected during a visit to the town of Butembo, one of the epicentres of the epidemic.
On Thursday, Abedi told The Associated Press that a person who had contact with the man confirmed as the second case was receiving treatment after showing signs of the disease. It has not yet been confirmed whether this third person is indeed suffering from Ebola.
If confirmed, it could be the first transmission of Ebola in this outbreak inside Goma.
Goma had prepared for the arrival of Ebola for months by setting up hand-washing stations, making sure motor-taxi drivers did not share helmets, vaccinating 3,000 healthcare workers, and running an operational treatment centre since February.
The lakeside city is close to the Rwanda border and has an airport with flights to the capital Kinshasa, Uganda’s Entebbe and Ethiopia’s Addis Ababa.
Early this month, neighbouring Rwanda said it would step up border monitoring and urged its citizens to avoid “unnecessary” travel to the eastern DRC.
Three Ebola cases were confirmed in neighbouring Uganda a month ago, but no new cases have since been registered.
The WHO’s emergency declaration – the fifth in history – brought in millions of dollars in new pledges by international donors.
However, some health workers say besides resources a new approach is needed to combat misunderstandings in the community.
A toxic mix of active armed groups and deep-rooted mistrust of health officials among local communities has hampered efforts to halt the virus with nearly 2,500 cases registered so far, according to the DRC’s health ministry.
Unidentified attackers killed two Ebola health workers near Mukulia in North Kivu early this month, the latest in a string of assaults this year that have killed or injured dozens of responders.
Amid the unrest, healthcare workers have vaccinated some 160,000 people, especially front-line workers.
The vaccine, developed by pharmaceutical giant Merck, is experimental but is estimated to be 97.5 percent effective and, according to WHO, may protect a person for up to 12 months.
The world’s worst epidemic of Ebola, a haemorrhagic fever that can spread through bodily fluids, killed about 11,300 people in West Africa as it surged through Guinea, Sierra Leone, and Liberia from 2013 to 2016.