Traditional healers help doctors reach patients in Sierra Leone
In a country where most people visit healers, some are stepping in to bridge the trust gap between the old and the new.

Tonkolili district, Sierra Leone – Slipping through a gap in the wooden perimeter fence that surrounds the Mabai Village Medical Clinic, Adama Kabia walks into the thick bushes, bending low in search of the herbs she needs to prepare her traditional medicines.
She carefully selects those she wants, moving plants aside one by one. Before long, she returns through the fence with a handful of healthy-looking green leaves.
Keep reading
list of 4 itemsDeadly Sahel heatwave caused by ‘human-induced’ climate change: Study
Woman, seeking loan, wheels corpse into Brazilian bank
UK set to ban tobacco sales for a ‘smoke-free’ generation. Will it work?
Back in the clinic garden, she walks over to a small iron pot on the floor, puts the leaves inside and starts beating them confidently. The muscle memory of more than 20 years of practice shows.
When she is finished, without hesitation, she pulls up her red top and rubs the mixture onto her left breast. “You apply it like this,” she says with an air of clinical distance.
“Leaves can help with gonorrhoea, dysentery, bloody diarrhoea. I saw men, women, and children with lots of different problems, but I specialised in speeding up pregnant women’s deliveries,” the 49-year-old explains.
She is one of about 45,000 traditional healers in Sierra Leone, a country that only has about 1,000 trained doctors, nurses, and midwives.
Adama’s practice of “Bulumba”, as herbal medicine is called in this region, brought her a steady income for many years. As a herbalist and healer, she is a trusted pillar in her community.
But almost six years ago, the Ebola outbreak changed everything.
Banned during the Ebola epidemic
October 2014. News about a deadly sickness had been circulating – it was spreading towards Tonkolili – the district in the northern province where Adama lives.
People were dying, many of them, her neighbours would tell each other.
Adama was sitting in her grey brick house after a long day. As usual, her porch radio was on. Her ears pricked at an announcement: An emergency decree from the government that all traditional healer practices must end.
She was shocked. Healing was her main source of income; her identity and standing in the community depended on it.
But traditional healers like Adama were now being blamed for the spread of Ebola; they were told they were hurting, not healing, the people around them.

Ebola first came to Sierra Leone in May 2014 after first reaching its neighbours Guinea and Liberia. Its impact on the country proved devastating. Of the 8,706 confirmed cases of Ebola there, 3,956 people did not survive the virus.
Although Adama herself stayed healthy, many healers died after interacting with Ebola patients, or contributed to the spread of the virus by passing it on to those they treated. At the height of the epidemic, patients would continue to seek care from local healers. The government tried to put an end to this.
“We found out that we would be held responsible for deaths and prosecuted,” Adama recalls. She says she accepted it in “good faith” as she was afraid of the consequences, but her livelihood was upended. She had to find another way to make a living. Gardening, as well as searching for gold in a nearby river, helped her to provide for her family.
Ebola gave Adama her first insight into the reality that there were things she could not and perhaps should not be treating with traditional herbs.
But as time passed, Ebola also drew the authorities’ attention to the reality that Sierra Leone’s medical system could not afford to completely exclude traditional healers. Their strong roots in society were a valuable asset.
Healers like Adama would later be brought in by authorities and medical professionals to spread awareness among their communities about how to combat the virus.
Adama’s new role
Despite the collaboration between modern medical professionals and some traditional healers during Ebola, there is still friction between the two camps.
Medics are often forced to deal with the life-threatening consequences of some traditional practices. When herbs prove to be ineffectual in the treatment of potentially fatal diseases like malaria, or when untrained healers fail to identify the signs of complications during childbirth, people arrive at medical facilities in desperation – and it can sometimes be too late for treatment.
In the case of malaria, for example, when fever rages and severe complications arise, such as convulsions or anaemia, without medical intervention, loss of life is common.
While traditional healers may be more aware of the limits of their practices, many are frustrated by a growing threat to their livelihoods and culture as community trust in low-cost local clinics and modern practices build.
But in Tonkolili district a programme has been started that tries to bridge the gap.

The NGO Concern Worldwide found that when traditional healers joined them in spreading the message about how to prevent and treat malaria, it was more successfully received in local communities. With a trusted healer telling people to visit a clinic, many more people followed their advice.
And so Adama became one of a growing number of traditional healers that have been trained by the organisation to identify the symptoms of malaria, and to direct patients straight to the nearest clinic.
“Treatment is free, but most people don’t know that,” she says. “They think they cannot afford to go to a doctor.”
What started as an NGO campaign against malaria, has today been widened in scope, with a fresh focus on pregnant women and small children, for whom the country also provides free healthcare at the point of delivery.
With this message, Adama walks from door to door – once in the morning, and once in the evening – meeting and advising people in her own 500-inhabitant community, as well as in surrounding villages.
The route she walks most often takes her from her house, down a red-sanded dirt track, in the shadow of tropical vegetation. After eight minutes, her journey ends at the Mabai Clinic. Here, she talks to the medical staff about developments in the community, and often stays on as a traditional birth attendant to help with deliveries.
One of the women whose baby she helped to deliver is 23-year-old Mariatu, today sitting next to Adama in the clinic’s garden. Smiling warmly, she adjusts the bright patterned cloth that holds her four-month-old baby against her back.
Without Adama, neither Mariatu nor her child might be alive today.
“I found her in the street,” Adama remembers, looking at Mariatu. “Her condition was clear.” She knew it was Malaria. “Her feet and face were swollen, she could barely stand.”
Sitting at the side of the street, the heavily pregnant Mariatu told Adama that she did not have any money to go to the clinic and that she would get better by applying herbs anyway.
But Adama kept insisting, telling her that healthcare was free. She even went one step further. “I’ll come with you,” she offered.
Mariatu refused Adama’s advice three times before she finally agreed to follow the healer to the clinic.
A legacy of traditional healing
The reason for Mariatu’s doubts extends beyond financial concerns.
Mariatu herself had been informally practising herbal healing from a young age. “Since my grandmother was a traditional healer, she shared with me a lot of her teachings and her herbs. I believed that I would be healed through traditional medicine,” she says.
Mariatu’s first child, an eight-year-old son, had never needed treatment beyond what her own home remedies were capable of. “He was delivered at home. I wasn’t sick. My child was never sick. I didn’t experience this before.”
Even after Ebola killed her grandmother, Mariatu’s commitment to traditional medicine held firm. And after meeting Adama that day, she was conflicted by her family teachings.
“I remembered my grandmother, and I told Madam Kabia that I am not going because my own grandmother has taught me how to use the traditional medicine, so this is what I will use,” Mariatu says. “But she told me to forget about all those traditional medicines and go to the hospital because I had malaria.”

The medication she was given was new to Mariatu, but she saw how much more effective the pills were than what she had used before at home. “I am so happy that this old woman came to my aid. I don’t know what would have happened without her.”
Since giving birth, Mariatu can often be found at the clinic where the nurses treat her young baby’s asthma.
Unfortunately, though Mariatu had a positive experience here, people’s fears about having to pay for medical treatment is sometimes justified. Some health workers, although few in number, do ask patients to pay them directly to make up for their low salaries. And when hospitals run out of medicine, which happens regularly, the patient has to buy it from a nearby pharmacy.
These issues can prevent patients from getting the treatment they need.
Traditional healers are more accessible, often live closer, and prescribe cheaper alternatives: herbs, roots, and barks that are readily available in their surroundings.
Witch-guns and red chicken
Some of Adama’s colleagues who continue to practise their traditional craft, also offer more ritualistic techniques as treatment.
“One method is that the patient brings me a red chicken,” says Patrick, a healer we meet in the local offices of Concern Worldwide, not far from Adama’s home. Patrick’s eyes have a serious look, sunken deep into their sockets. Behind him a fan is blowing against the green-blue fabrics that stretch across the large window, shielding the room from the bright sun outside.
“I will kill the chicken and we all eat together. The patient and my family, sometimes the neighbours. Then, at night, I will have a dream, a vision, of how to treat the patient that we gave the sacrifice for,” he continues with caution.
Patrick does not like to give away his secrets. Wearing a green-pink striped Lacoste knock-off shirt, he does not exactly seem like the stereotypical shaman, but his desire to keep parts of his practice secret is strong.
Patrick’s colleague, Samuel, is less cautious. Dressed in a white football shirt and matching white trousers, his voice fills the room with joyful laughter.
Samuel will often take patients to the clinic right away, especially when someone shows symptoms of malaria. “I know now that there are cases that are above me. Illnesses that I cannot cure. But there are also illnesses that the hospital cannot cure,” he adds quickly. For example, a hospital would not know how to treat demons, nor how to remove the bullets from “witch-guns”, he goes on to explain.
“My brother had an affair with the wife of another traditional healer. I told him to stop because that can be dangerous. But he didn’t stop. And it didn’t take long until he got high fever. It was because the other healer had shot him with his witch-gun. But luckily, I know how to treat this and managed to remove all 46 bullets,” Samuel explains.
For decades, these ritual practices and herbal medicine have been the source of both Patrick and Samuel’s livelihoods. The spread of modern medicine, however, seems to have put an expiry date on their services, and healers like them are afraid.
The practice of including healers and creating a bridge between the world of medicine and tradition is not yet widespread. NGOs like Concern Worldwide, who have trained 100 healers in Sierra Leone, are in the minority.

But the success of these initiatives suggests there might be room to expand. Including the likes of Patrick and Samuel in the healthcare provision at the local clinics has improved the relationship between clinic staff and healers who take part.
“Sometimes they ask me to bring special herbs. For example to speed up the delivery of a baby,” says Patrick. “We are friends now with the doctors in the clinic.”
A new virus, a new challenge
In the coming months, these new relationships will be tested and the success of the efforts to win people’s trust will be put on trial.
News about a new virus, “corona”, is reawakening old wounds in the community. A large poster has been put up next to the entrance of Mabai’s clinic. “If you have fever, cough and difficulty in breathing go to the nearest hospital or call 117 right away,” it reads.
“Since we have heard about this new disease, people are becoming scared and they are shying away from the hospital,” Adama says. Similar to the Ebola epidemic, people are afraid to see doctors, and scared of catching COVID-19 in health facilities.
The government, health workers, NGOs, and traditional healers like Adama have continuously worked to win back people’s trust ever since Ebola. But this new virus sounds all too familiar to many in the local community.
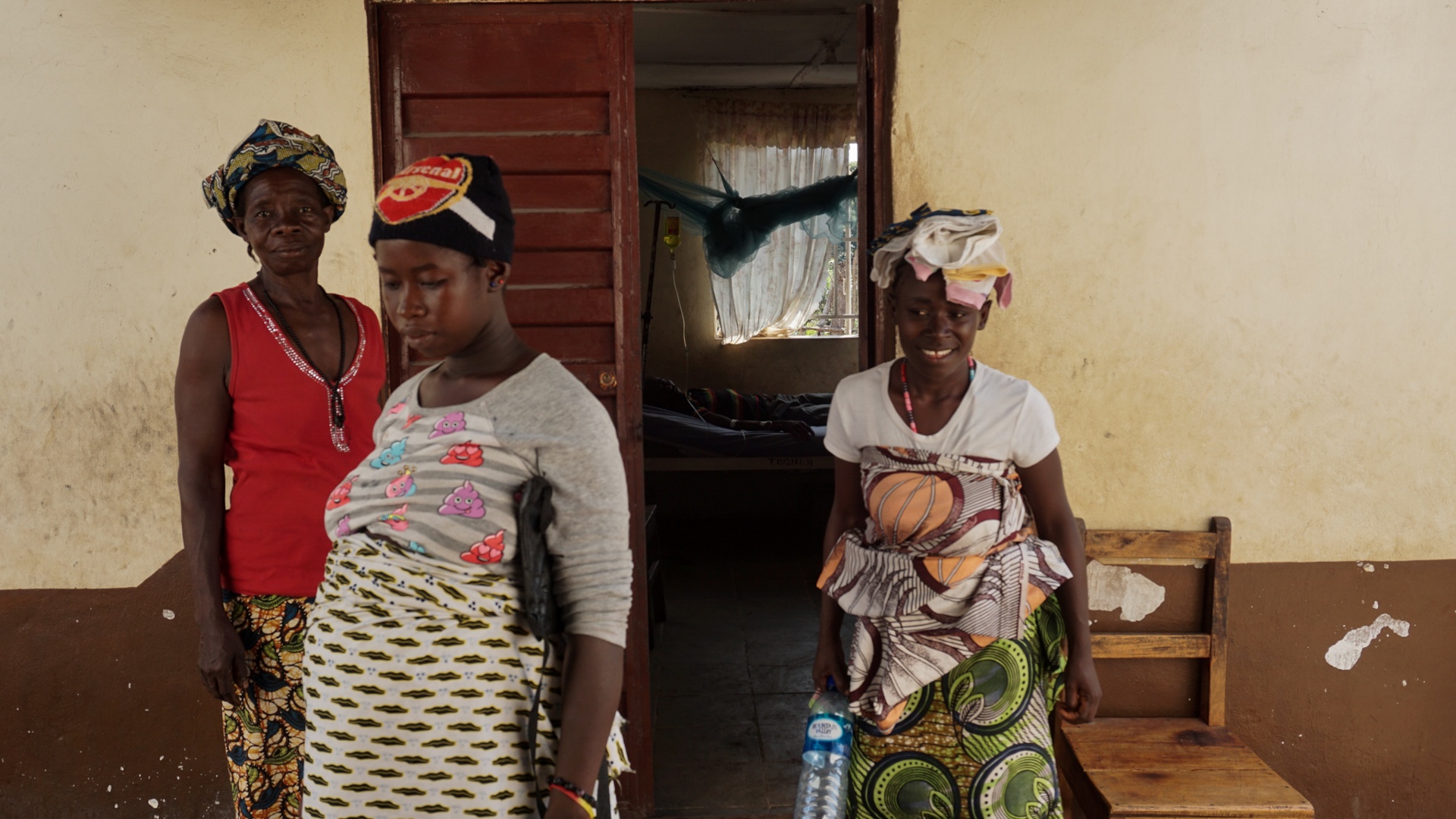
Adama is particularly worried that pregnant women and children under five will not be getting treatment when they need it. But she is working on that. “I have been talking to these women often, telling them not to shy away from the hospital, but to continue going to the hospital,” she says.
Whereas the Ebola outbreak brought a close to some of Adama’s herbal practices, when the government banned her work, today she feels included in the crisis response, she explains.
In the coming weeks, Adama will continue her community support role. Drawing on the lessons from her experience and her training, she hopes to make an impact.
“We, as traditional healers, know that there are diseases that should be treated traditionally and some that need to be taken to the hospital,” she says, before adding, “Corona is one to take to the hospital.”
This reporting was made possible by the European Journalism Centre’s Global Health Grant for Germany.