Ebola in the DRC: Everything you need to know
Key questions answered as another Ebola outbreak raises concern in the Democratic Republic of Congo.

New York City – This week, the World Health Organization (WHO) described the Ebola outbreak in Democratic Republic of Congo (DRC) as sitting on an “epidemiological knife-edge”.
According to government statistics released to Al Jazeera on Thursday, the total number of confirmed Ebola cases stands at 31. Authorities suspect a further 21 others as either probable or suspected cases of the viral disease.
Keep reading
list of 4 itemsWoman, seeking loan, wheels corpse into Brazilian bank
UK set to ban tobacco sales for a ‘smoke-free’ generation. Will it work?
Poland lawmakers take steps towards liberalising abortion laws
Though the Congolese government have only confirmed nine deaths thus far, there are suspicions that a total of 22 people may have already died from the virus.
Meanwhile, the WHO has shipped in thousands of doses of the vaccine to stem the virus from spreading. Other NGOs and aid agencies, like the medical charity Doctors without Borders (MSF), have stepped in build treatment facilities.
But health experts are concerned that the virus’ introduction to the city of Mbandaka, could usher in a new, possibly uncontrollable phase of the outbreak.
Here is everything you need to know about the virus in the DRC.
What is Ebola and where does it come from?
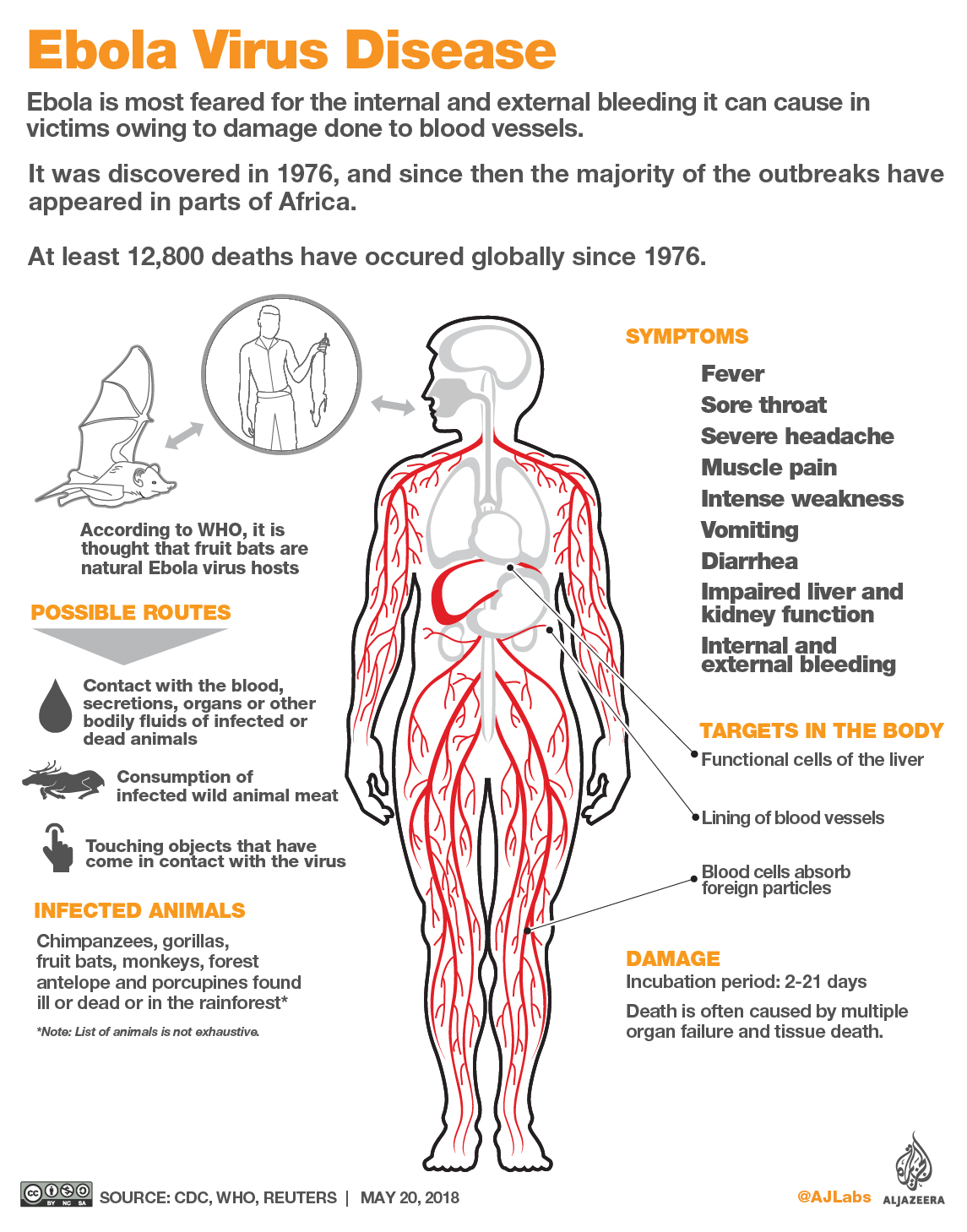
The Ebola Virus Disease (EVD) was first discovered in 1976 near the Ebola River in the DRC. It is considered a zoonotic virus, meaning that it originates from animals and is passed on to humans.
The virus causes a fever, cripples the cells that regulate blood pressure and causes organ failure.
Once infected, patients have a very low chance of surviving.
Symptoms include, but are not limited to fever, vomiting, diarrhoea, and internal and external bleeding.
Are there certain countries in the world more susceptible to Ebola?
The WHO describes Ebola as endemic to the DRC with the current outbreak being the ninth time the virus has made a significant appearance in the past 42 years.
“Ebola is introduced into the human population through close contact with the blood, secretions, organs or other bodily fluids of infected animals such as chimpanzees, gorillas, fruit bats, monkeys, forest antelope and porcupines found ill or dead in the rainforest,” Tarik Jasarevic, a spokesperson for the WHO based in Geneva, told Al Jazeera.
Similarly, Sterghios Moschos, a molecular biologist at the Northumbria University in Newcastle, England, told Al Jazeera that viruses like the Ebola virus or Nipah virus, which has claimed a dozen lives in India, often spring up among small animal populations faced with restricted movement.
“We simply don’t know where these viruses are hiding in the ‘jungle’, but they have been around probably for thousands of years … we only notice these viruses when they jump from animal to man and are able to transmit,” Moschos said.
When did the latest outbreak in the DRC begin?
The government of DRC declared an Ebola outbreak on May 8, 2018, after a series of suspected Ebola cases were reported to the ministry of health.
The ministry said two cases of the virus had been confirmed near the town of Bikoro in Equateur Province.
On May 17, the DRC government said the virus had reached Mbandaka, a city of 1.2 million, in what they cautioned could be “a new phase” of the virus.
|
|
However, Jessica Ilunga, communications officer for the DRC’s Ministry of Public Health, told Al Jazeera that the virus moving to Mbandaka, a city some 150km away from the original case, was not surprising.
“From the notification of the first cases in Bikoro, the government knew this would be a high-risk outbreak especially because Bikoro is near the city of Mbandaka. So Mbandaka was included in our response plan from the beginning,” Ilunga said.
But with Ebola moving to a transport hub situated on the Congo River, with direct access to Brazzaville, the capital of the Republic of Congo, and Bangui, the capital of Central African Republic, the possibility of the outbreak spiralling of control became a real possibility.
On Tuesday, EcoHealth Alliance, a research group that studies the intersection of animal, environment and human health, analysed flight patterns from airports in the region, and concluded that eight of out of the 10 cities most at risk from the current outbreak were African countries, with three inside the DRC alone.
Peter Daszak, president of the EcoHealth Alliance, told Al Jazeera from New York, that though neighbouring African countries should be most concerned, it is something that everyone in Europe and the US should be concerned about, too.
“Unfortunately, we (Americans) care about an outbreak only if it hurts us,” he said.
How have the DRC government and international community responded so far?
Many health experts and observers say that both local and international response has been swift. President Joseph Kabila managed to arrange $4m for the emergency response while the US pledged $7m to WHO’s call for assistance.
Ilunga from the Ministry of Public Health lauded the international community for being “more reactive and responding faster than in previous outbreaks”.
The WHO and the larger international community were severely criticised for failing to act promptly during the Ebola outbreak in West Africa between 2014-6.
According to Jasarevic from WHO, multiple partners are on board including the UN peacekeeping force in the DRC (MONUSCO) and the World Food Programme (WFP) to assist in reaching far-flung areas.
Some 4,500 doses of the vaccine have also been shipped to Mbandaka.
Congo’s Ministry of Public Health says vaccinations are an integral “part of the country’s response plan” and “a game changer”. Health workers in Mbandaka were first in line for the vaccine.
“Our surveillance teams on the ground have the important task of identifying and locating all the persons who have been in contact with confirmed Ebola cases in order to administer the vaccine and prevent them from developing the virus,” Ilunga said.
![Some 4,500 doses of the Ebola vaccine have been shipped to Mbandaka [Kenny Katombe/Reuters]](/wp-content/uploads/2018/05/fb456dece07e4637a1787ef2ff66647b_18.jpeg)
Others say that the Ebola outbreak points to a larger public health crisis in a country that is also home to a long-standing and underfunded humanitarian crisis.
Amakala Constantin Sodio, Catholic Relief Services’ (CRS) country representative in the DRC, told Al Jazeera that while the Ebola crisis was now “taking centre stage”, there was an urgent need for a renewed commitment to providing basic healthcare that would save lives in the country.
“Over time, and especially if Ebola isn’t contained quickly, it will strain the health system, [and] essential health services such as immunisation, prenatal care and safe births in health facilities will be negatively affected, and children will be at risk of dying in increasing numbers from preventable illnesses such as malaria and diarrhoea,” he said.
How does this outbreak compare to the one in West Africa in 2014?
The Ebola outbreak of 2014-6 in West Africa was the worst outbreak in the history of the virus.
Countries like Liberia, Sierra Leone and Guinea found themselves ill-equipped to deal with complex nature of the virus; nor were they able to handle patients and aftercare of victims.
The shortage of doctors and medical facilities, a difficult and deadly disease of which few knew the details about, mixed with a cascade of rumours and conspiracy theories combined for a most devastating cocktail. More than 11,000 people died.
Unlike the West Africa region, countries like the DRC and Uganda have significant experience with the disease.
Still, Moschos, from the University of Newcastle, says that conspiracy theories continue to “run wild about who and why these outbreaks keep happening”.
On Wednesday, three men infected with Ebola escaped from a health facility in Mbandaka. Two of the men later died, and the third was placed under observation, but the DRC authorities are desperately searching for others who might have come into contact with the men.
“At this point in time, distrust and misinformation is the greatest risk to the region, for this outbreak. We then have issues such as how care is given to ill people, religion, superstition and burial rites which help the virus transmit,” Moschos told Al Jazeera.
Moschos says the biggest difference between the outbreak in West Africa and the current one in the DRC is the record time in which “we have gone from discovering the outbreak to thousands of vaccines being delivered, money being made available, and everyone working together to tackle this.”
“The WHO has learnt the lessons from West Africa and the system is working. But we must engage the local people, not dictate them,” he said.
This time there is a vaccine. Is this the end of Ebola?
As it stands, there is no cure for Ebola. But a vaccine, now owned by American pharmaceutical company Merck, has been touted as the best chance to contain and control the spread of the virus.
The vaccine is still unlicensed and in an experimental stage but was used with much success in Guinea in 2015 and marks a dramatic departure from the methods of isolation and hygiene that characterised responses in the past.
At this point in time distrust and misinformation is the greatest risk to the region, for this outbreak
The vaccine is not without its challenges. For one, it requires refrigeration in areas where often there is little power.
Moreover, it is labour intensive. According to WHO, the process is not a once-off affair. The vaccination team have to visit all persons vaccinated on days three and 14 after the vaccination to monitor their well-being.
In terms of side effects, Moschos says that there is no evidence of any danger or dangerous side-effects emanating from the vaccine.
“There is a risk that the vaccine is not as effective as we believe and some people contract Ebola anyway. This risk is found with all vaccines, but here the stakes are higher,” he said.
“We need to show these people we feel the vaccine is safe, we need to show their leaders this, and we need their leaders to understand what is happening, and what is being done – in their own language,” Moschos said.
Follow Azad Essa on Twitter: @AzadEssa